[IMAGE PLACEHOLDER — FEATURED]
Alt text: Person massaging the heel of their foot to relieve plantar fasciitis pain
Concept: A person sitting on the edge of a bed, hands wrapped around their heel and arch in soft natural light. Relatable, not clinical.
That sharp pain in your heel when you take your first step out of bed is one of the most recognizable signs of plantar fasciitis. It shows up suddenly for some people and creeps in slowly for others, but the pattern is usually the same. The first few steps in the morning are the worst. The pain eases as you move around. Then it returns after long periods of sitting or standing.
Plantar fasciitis is the most common cause of heel pain in adults, and the good news is that most cases improve with the right combination of rest, stretching, and conservative care. Here is what is happening, why it happens, and what to do about it.
What plantar fasciitis is
The plantar fascia is a thick band of tissue that runs along the bottom of your foot, connecting your heel bone to your toes. Think of it like a bowstring that supports the arch of your foot every time you take a step.
When that tissue gets overloaded, small tears form where it attaches to the heel. The tissue becomes inflamed and irritated. That irritation is what you feel as plantar fasciitis pain. According to the American Academy of Orthopaedic Surgeons, it is the most common cause of pain on the bottom of the heel.
Symptoms to watch for
Plantar fasciitis has a distinct pattern. The pain is usually located on the bottom of the heel or along the arch. Common signs include:
- Sharp, stabbing pain in your heel during your first steps in the morning
- Pain that improves once you start walking, then returns after long periods of standing
- A deep ache after exercise, not usually during
- Stiffness that flares up after sitting for a while
- Tenderness when you press on the bottom of your heel
[IMAGE PLACEHOLDER — INLINE 1]
Alt text: Diagram of the plantar fascia ligament along the bottom of the foot
Concept: Simple anatomical illustration of the foot from a side view, with the plantar fascia highlighted from heel to toes. Clean and educational.
What causes it
Plantar fasciitis is almost always an overuse injury. The tissue gets stressed beyond what it can recover from, and inflammation sets in. Some of the most common contributors:
- A sudden increase in activity, like ramping up your running mileage or starting a new job that keeps you on your feet
- Tight calf muscles or limited ankle flexibility
- Flat feet or very high arches that change how your foot absorbs impact
- Spending long hours on hard surfaces in unsupportive shoes
- Carrying extra weight, which increases the load on the plantar fascia
- Age. After 40, the tissue starts to lose elasticity, and plantar fasciitis becomes most common between ages 40 and 60
It is worth saying out loud: plantar fasciitis is not a sign that you did something wrong. It is the body's response to a load it cannot keep up with, and the fix is almost always about reducing that load while the tissue heals.
How to take care of it at home
Most people get meaningful relief within a few weeks of consistent self-care. The basics:
- Rest from the activity that triggered it. If running set it off, switch to swimming or biking until the pain settles.
- Ice the heel for 10 to 15 minutes two or three times a day, especially after activity.
- Stretch the calf and the bottom of the foot every morning before standing up. Rolling a tennis ball or frozen water bottle under your arch is a simple place to start.
- Wear supportive shoes with cushioning and an arch that fits your foot, even at home. Going barefoot on hard floors is one of the fastest ways to flare it up.
- Try over-the-counter inserts. They give the arch some help while the tissue settles down.
Anti-inflammatory medications like ibuprofen can reduce pain and swelling, but they are not a long-term plan. If you find yourself needing them every day, that is a signal to see a specialist.
When to see a doctor
Plantar fasciitis usually responds to conservative care, but there are clear signs it is time to bring in a specialist:
- The pain has lasted longer than four to six weeks despite home treatment
- It is severe enough to change how you walk
- The pain wakes you up at night, or you have numbness or tingling in the foot
- You felt a sudden pop or sharp tear during exercise
- You have diabetes, poor circulation, or a history of stress fractures
For Central Texas patients, BoneDrs offers evaluations across our Austin, San Marcos, Bastrop, Lockhart, and Round Rock locations.
Treatment options at BoneDrs
Dr. Arush Angirasa, our fellowship-trained foot and ankle specialist, sees patients with plantar fasciitis at every stage. The vast majority of cases never need surgery, and our approach starts with the least invasive option that can resolve the problem.
Non-surgical options often include:
- A targeted stretching and strengthening program for the calf, Achilles, and small muscles in the foot
- Custom or semi-custom orthotics that support the arch and reduce strain on the fascia
- Night splints that hold the foot in a stretched position while you sleep
- Cortisone injections for cases where pain has not responded to several weeks of conservative care
- Referral for hands-on physical therapy
When pain has lasted six to twelve months and conservative care has not worked, surgical options become part of the conversation. Procedures like a partial plantar fascia release are reserved for severe, treatment-resistant cases. The goal is always to get you back to walking, working, and exercising without daily heel pain. You can learn more about our full range of conservative and surgical care on our sports medicine service page.
[IMAGE PLACEHOLDER — INLINE 2]
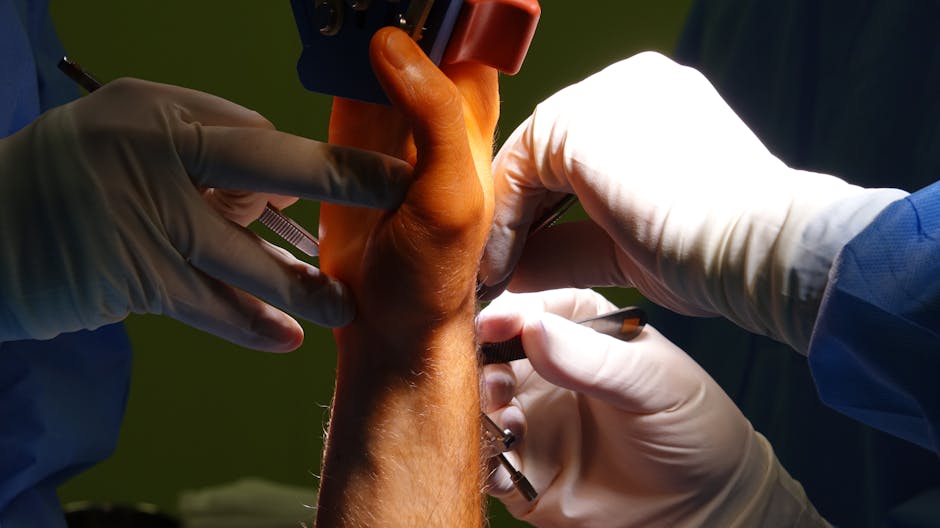
Alt text: Foot and ankle specialist examining a patient's heel during an appointment
Concept: Provider hands examining a patient's foot in a clinical exam room. Approachable and warm, no graphic imagery.
Recovery timeline
Most patients see noticeable improvement within four to eight weeks of starting consistent treatment. According to Mayo Clinic, full recovery can take several months, especially if the condition has been ignored for a while. The pattern usually looks like this:
- Weeks 1 to 4: Sharper morning pain begins to ease with daily stretching and activity changes
- Weeks 4 to 8: Pain becomes less frequent, and longer activity becomes possible again
- Months 2 to 6: Most people return to full activity, with continued stretching as a maintenance habit
The biggest mistake we see is patients pushing back into full activity the moment the pain fades. Healing tissue still has to be strong enough for impact, and ramping up too fast is the most common reason plantar fasciitis comes back.
Frequently asked questions
Will plantar fasciitis go away on its own?
Many cases improve with consistent home care, but ignoring it makes recovery longer. If pain has lasted more than four weeks, getting evaluated early shortens the path back to normal activity.
Can I keep running with plantar fasciitis?
Most specialists recommend reducing or pausing high-impact activity until the pain has eased significantly. Switching to swimming, cycling, or the elliptical lets you stay fit while the tissue heals.
Are heel spurs and plantar fasciitis the same thing?
No. A heel spur is a small bone growth on the heel that often shows up on imaging, but most heel spurs are not painful on their own. Plantar fasciitis is the inflammation of the soft tissue, and that is usually what is causing the pain.
Schedule a consultation at BoneDrs
If your heel pain is not improving on its own, a foot and ankle specialist can shorten the path back to walking pain-free. Call 512-266-3377 to schedule a visit at any of our five Central Texas locations.
If you have any concerns about your joints, contact us and we can help determine a treatment that works for you.