Understanding Your Jones Fracture: What You Need to Know

A non displaced jones fracture is a break in the fifth metatarsal bone at the base of your foot, specifically at the junction where the bone shaft meets the growth plate (Zone 2). Unlike a displaced fracture, the bone pieces remain aligned, which often allows for non-surgical treatment options.
Key Facts About Non Displaced Jones Fractures:
- Location: Zone 2 of the fifth metatarsal (the long bone on the outside of your foot)
- Symptoms: Pain, swelling, bruising on the outer edge of your foot, difficulty walking
- Non-Surgical Treatment: 6-8 weeks of immobilization in a cast or walking boot
- Success Rate: 72-93% union rate with proper conservative management
- Risk: 15-30% chance of nonunion due to limited blood supply in this area
- Recovery Timeline: Typically 3-4 months to full activity
This type of fracture is particularly challenging because it occurs in a vascular watershed area—a region with limited blood supply that makes healing slower and less predictable than other foot fractures.
The good news? Many patients, especially those who aren't competitive athletes, can heal successfully without surgery. Treatment typically involves strict immobilization and limiting weight-bearing activities while your bone repairs itself.
As Christopher Jimenez, MD, a board-certified orthopedic surgeon specializing in lower extremity trauma and fractures in the Central Texas region, I've successfully treated numerous patients with non displaced jones fractures using both conservative and surgical approaches. My experience across our Austin, San Marcos, and Bastrop locations has shown that the right treatment path depends on your activity level, healing progress, and personal goals.
Understanding the Jones Fracture: More Than Just a Broken Bone
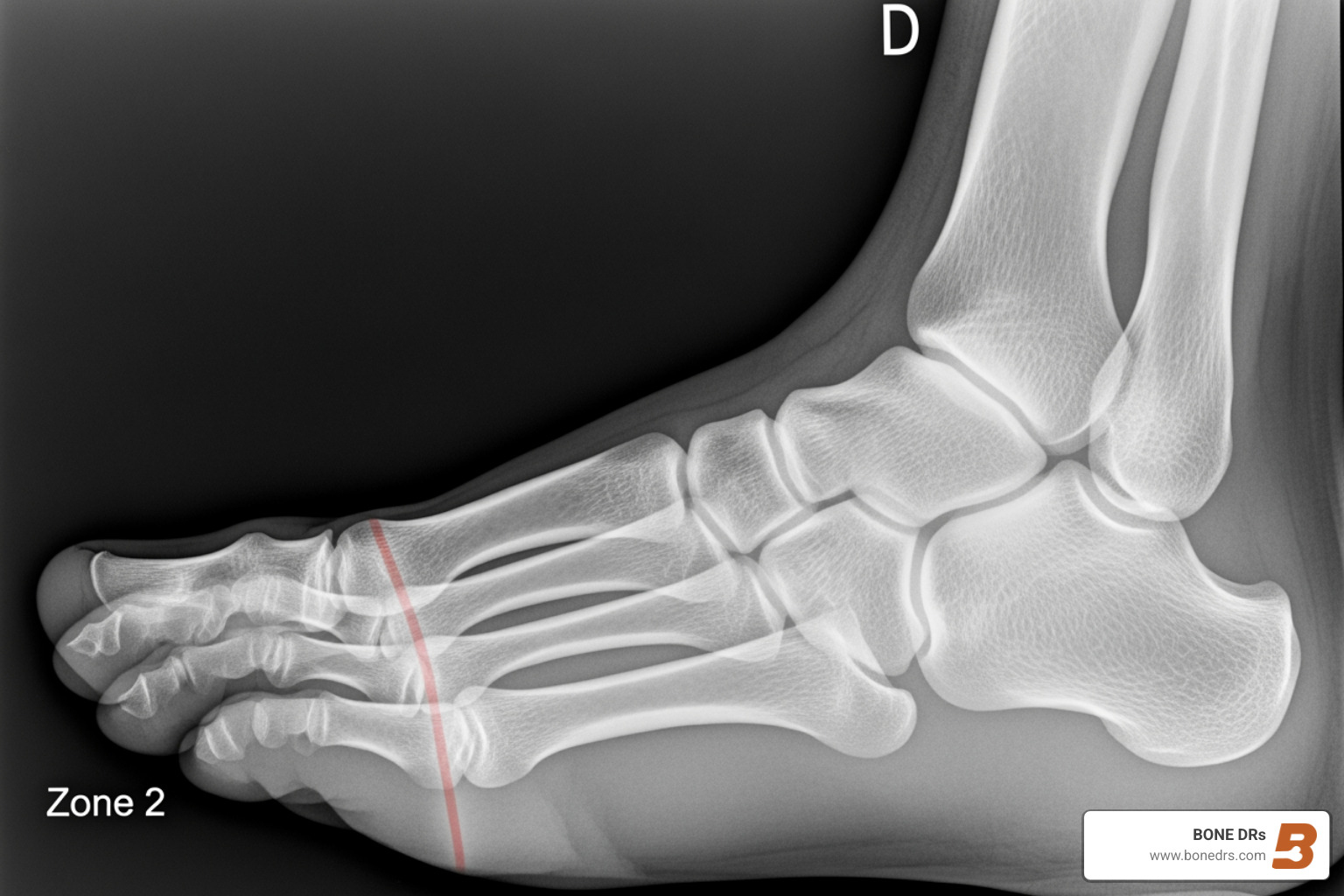
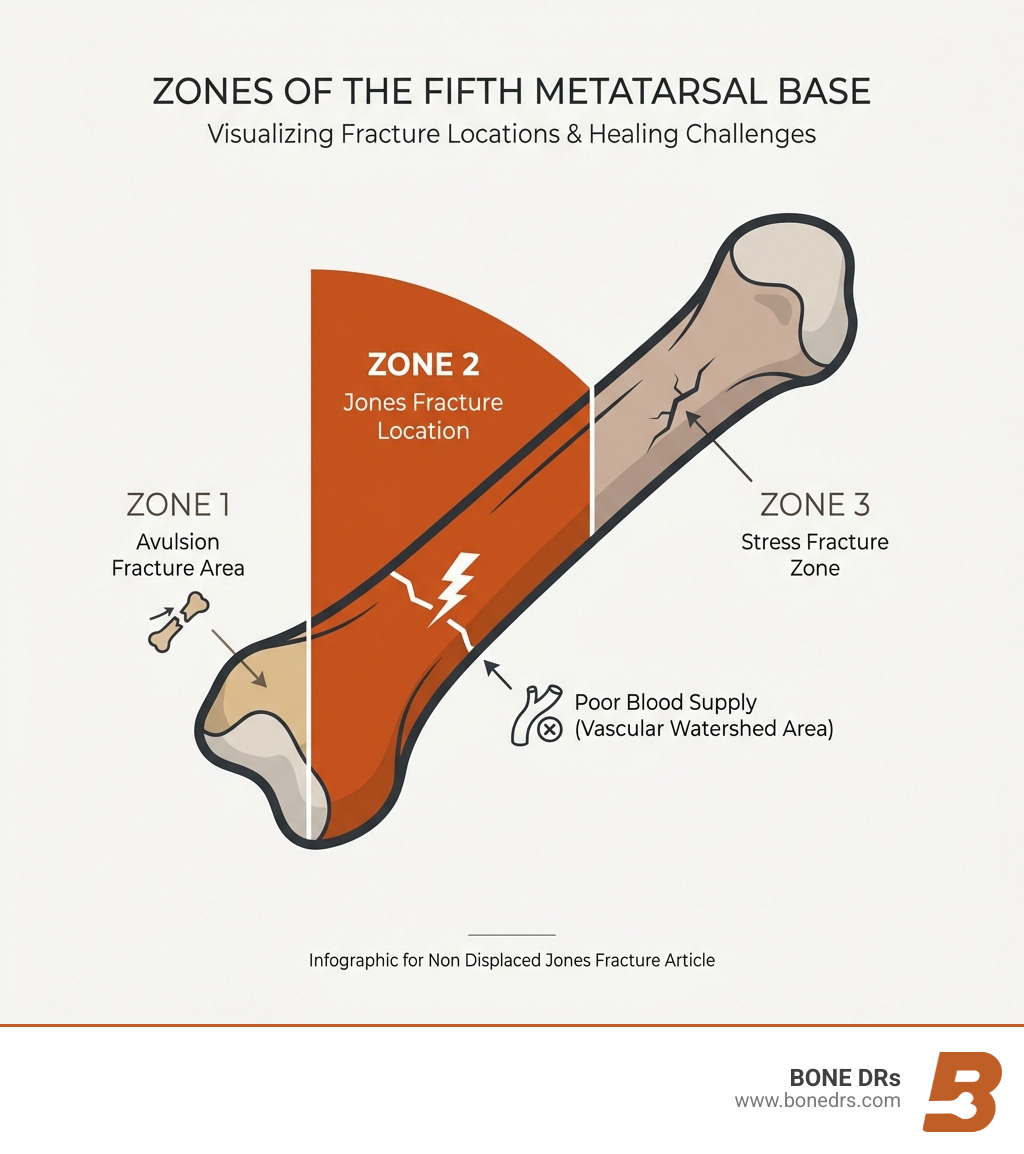
A Jones fracture is a break at the metaphyseal–diaphyseal junction (Zone 2) of the fifth metatarsal—just beyond the bony bump you can feel on the outside of your foot. What makes Jones fractures unique is the limited blood supply at this location. That’s why even a “clean,” aligned break can take longer to heal and sometimes fails to unite without careful management.
Common symptoms include:
- Sharp pain and pinpoint tenderness over the outer midfoot
- Swelling and bruising along the lateral foot
- Difficulty or inability to bear weight
- Pain that worsens with push-off or twisting
If you’re feeling these symptoms, don’t power through. An X-ray is the first step. In some cases, an MRI or CT can help when X-rays are unclear or if healing takes longer than expected. Learn more about foot fractures and how we diagnose them here: More info about Foot Fracture.
Differentiating Jones Fractures
Not all fifth metatarsal fractures are the same:
- Pseudo-Jones (Zone 1) avulsion fracture: A chip of bone is pulled off the base of the fifth metatarsal, usually from a sudden inversion injury. These typically heal well with a stiff-soled shoe or boot.
- Jones fracture (Zone 2): The true Jones fracture at the metaphyseal–diaphyseal junction. This is the one with a higher risk of nonunion.
- Zone 3 stress fracture: A more distal, diaphyseal stress injury that can have an even longer healing course (sometimes up to 20 weeks).
Mechanism of injury often involves an adduction force to the forefoot with the ankle in plantar flexion—think a misstep, a twist while pivoting, or an awkward landing.
The Conservative Approach: Treating a Non Displaced Jones Fracture Without Surgery
When the fracture is non-displaced (aligned) and you’re not a high-performance athlete, conservative management is usually our first choice. Why? Because it works for most people—and it avoids surgical risks.
Core goals of non-surgical care:
- Keep the fracture absolutely still so bone can bridge the gap
- Protect the area from repetitive stress
- Control swelling and pain
- Return you safely to activity
The Role of Immobilization: Cast vs. Walking Boot

Immobilization is the star of the show. We’ll typically use either a short leg cast or a CAM (controlled ankle motion) boot.
Cast vs. Boot: Pros and Cons
- Cast (usually non-weight-bearing for 6-8 weeks)
- Pros:
- Superior immobilization and compliance (you can’t remove it)
- Historically high union rates for Jones fractures (72-93% reported for NWB casting)
- Cons:
- No showering without covers
- Muscle atrophy and ankle stiffness are more common
- Daily life disruptions and fall risk with crutches
- Pros:
- Walking Boot (weight-bearing can vary by plan)
- Pros:
- Removable for hygiene and gentle, provider-guided motion later in recovery
- Easier for daily living and sleep comfort
- Often similar outcomes in carefully selected patients
- Cons:
- Success depends on your compliance—taking it off too much can delay healing
- Not ideal for elite or high-demand athletes
- Pros:
What does the latest evidence suggest? In a case series of adults with acute Jones fractures, patients allowed to walk as tolerated in a boot had mostly good outcomes—66.7% showed radiographic union, and others were pain-free despite partial union. Only 3 out of 47 (6.4%) in the weight-bearing-as-tolerated (WBAT) group needed surgery, compared with 3 out of 8 (37.5%) in the strict non-weight-bearing (NWB) cast group. That suggests functional treatment in a boot can work well for low-demand adults—but it’s not a one-size-fits-all approach. We’ll tailor your plan after examining your fracture pattern, your goals, and your lifestyle.
Who is a Good Candidate for Non-Surgical Treatment?
We generally recommend a conservative plan if you:
- Have a clearly non-displaced Zone 2 (Jones) fracture
- Are a low-demand individual or recreational athlete
- Can commit to wearing your boot or cast exactly as prescribed
- Prefer to avoid surgery and accept a bit longer healing timeline
- Do not need a rapid return to cutting/pivoting sports
- Do not show risk factors that push us to surgery (for example, a painful nonunion developing, progressive displacement, or repeated refracture)
If you’re an elite athlete or your job demands rapid, predictable return to high-impact activity, surgery may be the more reliable route.
Expected Recovery Timeline for a non displaced jones fracture
- Weeks 0-2: Strict immobilization in a cast or boot. Most patients remain non-weight-bearing or toe-touch weight-bearing initially. Elevation is your friend.
- Weeks 3-6: Continue immobilization. Depending on pain and X-rays, we may allow partial weight-bearing (boot only) and start gentle ankle range of motion that doesn’t stress the fracture.
- Weeks 6-8: Follow-up imaging. Many patients transition to progressive weight-bearing in the boot. If healing is on track, we plan a gradual return to shoe wear with a stiff insert.
- Weeks 8-12+: Physical therapy to restore strength, balance, and calf/ankle mobility. Return to full activity tends to occur between 3-4 months, but we read the bone, not the calendar.
We’ll verify radiographic union (bone bridging on X-rays) as a green light. Some studies note radiographic union around 16 weeks on average. Don’t worry if your progress is slightly faster or slower—healing is personal.
Outcomes and Potential Complications of Non-Operative Treatment
The big question: “Will it heal?” For non-displaced Jones fractures treated without surgery, published union rates range from 72% to 93% when strict casting and non-weight-bearing are used. In select low-demand adults treated functionally in a boot, outcomes can be satisfactory too, with many patients achieving either radiographic union or becoming pain-free even if a partial union persists.
You can review an overview of diagnostic and treatment considerations here: Latest research on Jones fracture treatment.
A few other data points to keep in mind:
- Nonunion rates for Zone 2 (Jones) fractures are reported as high as 15-30%, mainly due to the poor blood supply at this location.
- Refracture can occur after cast or boot removal if you ramp activity too fast or return to impact sports before the bone is ready.
- Zone 3 stress fractures (not Jones fractures) may take up to 20 weeks to heal, which is one reason we’re careful when symptoms are chronic or there’s significant sclerosis on imaging.
If you have persistent foot pain during or after treatment, we’ll reassess and support you with a plan. Learn more about managing ongoing symptoms here: Learn about managing persistent Foot Pain.
Risks of Conservative Management
No treatment is risk-free, even when it’s “non-surgical.” Key risks include:
- Nonunion (15-30% risk in Zone 2 injuries)
- Delayed union (healing that takes longer than expected)
- Refracture after immobilization ends (especially if return to impact is too fast)
- Chronic pain or weakness if rehab is skipped or rushed
How we lower those risks:
- We individualize your weight-bearing plan based on pain and imaging
- We monitor your healing with follow-ups so we can adjust treatment early
- We address contributing factors like varus alignment or poor footwear support
- We guide your return to activity and sport with a phased, criteria-based plan
When is Surgery the Right Choice?
Surgery can be the right tool for the job if you need a faster, more predictable union—especially for high-demand athletes—or if the bone simply isn’t healing with conservative measures. Typical surgical treatment for a Jones fracture involves intramedullary screw fixation, sometimes with biologic augmentation for nonunion cases. Union rates with modern surgical techniques are very high in experienced hands.
Key Indications for Surgical Intervention for a non displaced jones fracture
We talk seriously about surgery if:
- You’re an elite or competitive athlete who needs a reliable, faster return to sport
- Painful nonunion develops despite appropriate immobilization
- The fracture displaces on follow-up imaging
- You’ve had a refracture
- You prefer a surgical solution after understanding risks and benefits
Curious about what surgery entails and whether it’s right for you? Explore options with us: Explore Jones Fracture Surgery options.
Frequently Asked Questions about Non-Surgical Jones Fracture Treatment
How long will I be in a boot or cast?
Plan on 6 to 8 weeks of immobilization. Some patients will need longer (especially if pain persists or imaging shows slow progress). We’ll check follow-up X-rays to confirm healing and adjust your plan accordingly.
Can I walk on a non-displaced Jones fracture?
It depends on your fracture specifics and our shared plan. Traditional guidance for Jones fractures favors non-weight-bearing for 6-8 weeks to reduce the risk of nonunion. In low-demand adults, carefully selected patients may do well with weight-bearing as tolerated in a walking boot under close supervision. The key is strict immobilization and not pushing through pain. If we advise non-weight-bearing, it’s for a reason—protect the repair.
What is the nonunion rate for a non-displaced Jones fracture?
Even when everything goes right, the anatomic location of a Jones fracture carries a 15-30% nonunion risk. That’s why compliance with the plan—and timely follow-ups—matters. If nonunion occurs, we’ll discuss the best next step, including surgical options with excellent success rates.
Your Path to Recovery and a Return to Activity
Our approach at BONE DRs Orthopedic Care is simple: personalize your plan, protect your healing, and guide you back to what you love—safely. For many patients with a non displaced jones fracture, a non-surgical path is not only possible but preferable. We’ll partner with you to:
- Choose the right immobilization (cast or boot)
- Decide the safest weight-bearing strategy
- Monitor healing with the right cadence of follow-ups
- Rebuild strength and balance with smart rehabilitation
- Prevent setbacks with footwear, orthotics, and training guidance
We provide comprehensive Foot & Ankle care across Austin, North Austin, San Marcos, and Bastrop. If you’re dealing with a new fracture—or persistent pain after an injury—let’s talk. We can often see you promptly and start the right plan on day one.
- Learn how we manage injuries like yours: More info about Fractures & Trauma care
- Meet our team and get specialized care: Consult with our Foot and Ankle specialists
We’re here to help you step forward confidently—one careful step at a time. And yes, we’ll remind you to wear your boot. Even to the fridge.
If you have any concerns about your joints, contact us and we can help determine a treatment that works for you.