Understanding Jones Fractures: What You Need to Know

A jones fracture is a break in the fifth metatarsal bone—the long bone on the outer edge of your foot, just behind your pinky toe. This specific fracture occurs near the base of the bone where blood supply is naturally limited, making it notorious for slow healing and high rates of complications.
Quick Facts About Jones Fractures:
- Location: Base of the fifth metatarsal (outer foot bone)
- Common Symptoms: Sharp pain on outside of foot, swelling, bruising, difficulty walking
- Healing Time: 6-12 weeks with proper treatment
- Key Challenge: Poor blood supply leads to nonunion in up to one-third of cases
- Risk Factors: Athletes, sudden direction changes, high-impact activities
- Treatment Options: Non-surgical immobilization OR surgical screw fixation
Unlike other foot fractures that heal predictably, Jones fractures occur in what doctors call a "watershed area"—a zone where blood vessels don't reach well. This anatomical reality explains why these injuries often frustrate both patients and physicians. The fracture was first described in 1902 by Sir Robert Jones, an orthopedic surgeon who ironically broke his own foot while dancing.
Athletes face particularly high risks, with males experiencing these fractures ten times more often than females. Basketball players, dancers, and soccer players frequently encounter this injury when pivoting, jumping, or making sudden lateral movements.
As Christopher Jimenez, MD, a board-certified orthopedic surgeon specializing in lower extremity trauma, I've treated countless patients with Jones fractures throughout Central Texas. My training in minimally invasive techniques and focus on evidence-based care helps patients understand their options and achieve the best possible outcomes for these challenging injuries.

Anatomy, Causes, and Symptoms of the Jones Fracture
To understand why a jones fracture is so troublesome, we have to look at the unique "geography" of the fifth metatarsal. This bone is a long, slender structure on the lateral (outer) side of your foot. It serves as a major attachment point for several tendons and ligaments that help you balance and move.
The primary reason this fracture is a "problem child" in orthopedics is the watershed area. In medical terms, a watershed area is a region that sits between two different blood supply sources but doesn't get a robust flow from either. When you break a bone, it needs blood—which carries oxygen and nutrients—to knit back together. Because the base of the fifth metatarsal has such a finicky blood supply, the healing process is often stalled.
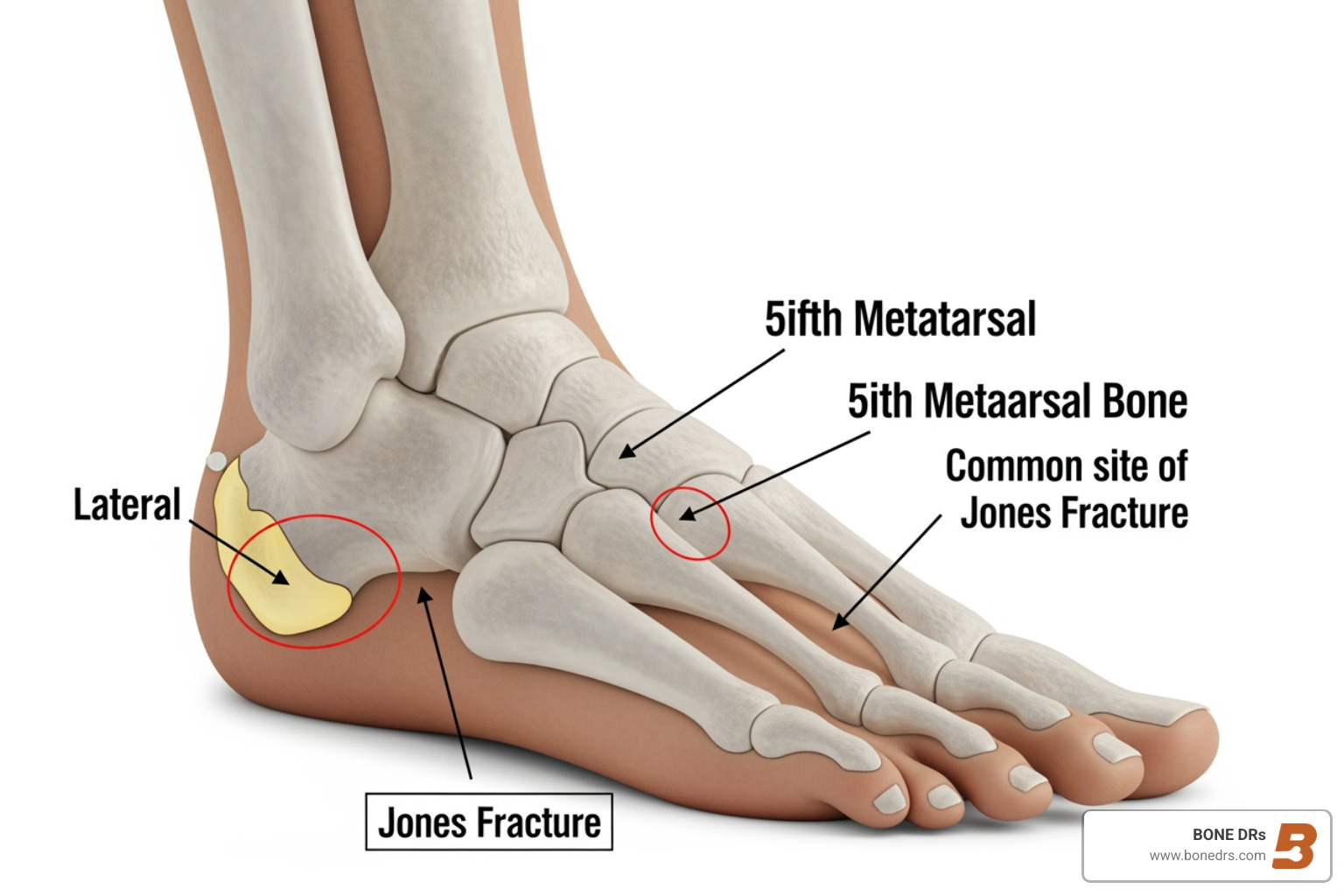
Common Causes and Mechanisms
Most jones fracture injuries happen during "indirect violence" to the foot. This isn't a scene from an action movie; it usually involves:
- Lateral Movement: Sudden side-to-side cutting motions common in tennis or basketball.
- Rolling the Ankle: An inward twist of the foot while the toes are pointed down.
- Overuse: Repetitive stress that creates a small crack which eventually snaps.
- Changing Direction: Pivoting with your heel off the ground.
Identifying the Symptoms
If you’ve sustained a jones fracture, you likely won't be able to "walk it off." Common signs include:
- Sharp Pain: Intense pain localized on the outside of the midfoot.
- Swelling and Tenderness: The area will likely be puffy and very painful to the touch.
- Bruising: Discoloration often appears shortly after the injury.
- Difficulty Walking: Most patients find it nearly impossible to bear weight on the outer edge of the foot.
For a deeper dive into the science behind these injuries, you can explore this Scientific research on 5th metatarsal fractures. If you are experiencing general discomfort, check out our More info about foot pain page.
Anatomical Zones of the Fifth Metatarsal
Not all breaks in this bone are created equal. Surgeons divide the base of the fifth metatarsal into three distinct zones to determine the best treatment:
- Zone 1 (Avulsion Fracture): This happens at the very tip of the bone. It’s often called a "pseudo-Jones" or "dancer's fracture." A tendon pulls a small piece of bone away. These usually heal well with a simple walking boot.
- Zone 2 (The true Jones Fracture): This occurs at the metaphyseal-diaphyseal junction. This is the "danger zone" where the blood supply is poorest.
- Zone 3 (Stress Fracture): This is further down the shaft. These are almost always caused by repetitive stress rather than a single injury and are common in elite athletes.
Doctors also use the Torg classification to describe the "age" of the fracture. A Type I is a fresh, acute break. Type II shows signs of delayed healing (widened fracture line), and Type III is a nonunion where the bone has essentially stopped trying to heal itself.
Why Athletes are at Higher Risk for a Jones Fracture
In the athletic world, the jones fracture is a well-known foe. Statistics show that in athletes, these fractures are 10 times more likely to occur in males, with a mean age of 26.
Why are athletes targeted?
- High-Impact Sports: Basketball, soccer, and football involve constant pivoting and explosive lateral movements.
- Foot Alignment: Individuals with cavovarus feet (high arches) put significantly more pressure on the outside of their feet, making them prime candidates for Zone 2 and 3 fractures.
- Training Surfaces: Playing on hard surfaces or artificial turf increases the stress transmitted to the fifth metatarsal.
For more technical insights, you can read the Research on Jones fractures in athletes.
Diagnosis and Classification Systems
When you come into one of our BONE DRs locations in Austin or San Marcos, our first goal is to distinguish a jones fracture from its less-serious cousins.
The diagnostic process typically involves:
- Physical Exam: We check for point tenderness over the base of the fifth metatarsal and test your ability to bear weight.
- X-rays: This is the gold standard. We take views from the front (AP), side (lateral), and at an angle (oblique). We look for the fracture line and any signs of sclerosis (bone hardening) that might suggest it’s an old injury that didn't heal.
- MRI or CT Scan: If the X-ray is inconclusive but you still have pain, an MRI can pick up "bone edema" (swelling inside the bone). A CT scan is excellent for seeing if the bone has achieved medullary obliteration—where the internal canal of the bone is blocked by scar tissue, preventing healing.
Correctly identifying the Torg Type (I, II, or III) is critical. A Type I fracture might be a candidate for a cast, but a Type III nonunion almost always requires surgery. Learn more about how we handle these cases on our More info about foot fractures page.
Treatment Options for a Jones Fracture
Deciding how to treat a jones fracture involves a conversation about your lifestyle. Are you a collegiate athlete who needs to be back on the field in two months, or are you a casual walker who doesn't mind a slower pace?
| Feature | Non-Surgical Treatment | Surgical Fixation |
|---|---|---|
| Method | Cast or Boot + Crutches | Screw or Plate Placement |
| Weight Bearing | Strict non-weight bearing (6-8 weeks) | Earlier protected weight bearing |
| Healing Rate | ~66-75% success | ~97% success |
| Return to Sport | Average 13-15 weeks | Average 7-9 weeks |
| Risks | High nonunion/refracture risk | Infection, hardware irritation |
Non-Surgical Management
For non-athletes with a "clean" (nondisplaced) fracture, we may recommend:
- Strict Non-Weight Bearing: Using crutches and a short leg cast for at least 6 weeks.
- Walking Boots: Transitioning to a boot once early healing is seen on X-ray.
- Bone Stimulators: These devices use ultrasonic or electrical currents to "jump-start" bone cells in the watershed area.
However, be aware that up to 50% of Jones fractures may not heal with casting alone. If progress isn't seen by week six, we often pivot to surgical options. Explore our More info about minimally invasive foot surgery for more details.
Surgical Fixation Techniques
Surgery is often the preferred route for athletes and active individuals because it provides internal stability and increases the success rate to nearly 97%.
- Intramedullary Screws: This is the most common technique. We place a single, solid screw down the center of the bone to "compress" the fracture. Using a larger diameter screw (4.5mm or larger) is often preferred to prevent the screw from breaking.
- Plantar Plates: If the bone is too small or the fracture is too complex for a screw, we use a specially contoured plate on the bottom (plantar) side of the bone.
- Cannulated Screws: These are hollow screws placed over a guide wire, allowing for extreme precision with smaller incisions.
- Bone Grafting: For chronic nonunions, we may take a small amount of "bone " (either your own or from a donor) to fill the gap and stimulate new growth.
For those considering the surgical route, see More info about Jones fracture surgery.
Recovery and Rehabilitation Protocol
Recovery from a jones fracture is a marathon, not a sprint. Even with a successful surgery, the bone needs time to solidify.
The 5-Phase Rehab Protocol
We typically follow a structured rehabilitation path:
- Phase 1 (Weeks 0-2): Healing and Protection. Strict non-weight bearing. Focus on reducing swelling.
- Phase 2 (Weeks 2-4): Protected Weight Bearing. Toe-touch weight bearing in a boot.
- Phase 3 (Weeks 4-6): Strengthening. Starting range-of-motion exercises and light resistance bands.
- Phase 4 (Weeks 6-10): Functional Activities. Transitioning to regular shoes. Aquatic therapy is a fantastic way to regain strength without putting full body weight on the bone.
- Phase 5 (Weeks 10+): Return to Play. Sport-specific drills and agility training.
For athletes, the goal is a safe return to competition. Research shows that surgical fixation allows for an early return to play, often around the 8-to-10-week mark, compared to 13+ weeks with a cast.
Frequently Asked Questions
Why is a Jones fracture so hard to heal?
It all comes down to the watershed area. The base of the fifth metatarsal has very poor vascularity (blood flow). Additionally, the powerful fibularis brevis tendon attaches right near the fracture site and constantly pulls on the bone, which can prevent the two ends from staying together long enough to knit. This leads to a nonunion rate of about 33% in non-surgical cases.
Can I walk on a Jones fracture?
No. Walking on an undiagnosed or fresh jones fracture can displace the bone further and virtually guarantee it won't heal. Expect to be on crutches or a knee scooter for 6 to 8 weeks. Even "protected weight bearing" usually doesn't start until we see signs of new bone growth on an X-ray.
How long does surgery recovery take?
While every patient is different, athletes often achieve clinical union in about 7.5 weeks post-surgery. Most patients return to "normal life" activities within 3 to 4 months. The use of a solid intramedullary screw significantly reduces the time you have to spend completely off your feet.
Conclusion
A jones fracture is a serious injury that requires expert management to avoid long-term foot problems. Because of the limited blood supply in the fifth metatarsal, "wait and see" is rarely the best strategy, especially for active residents in the Austin area.
At BONE DRs, we take a multidisciplinary approach to your care. Whether you need a custom-molded cast and a bone stimulator or a precision-placed intramedullary screw, our board-certified specialists are here to guide you. We serve patients across Austin, San Marcos, Bastrop, and Lockhart, ensuring that high-quality orthopedic care is always close to home.
Don't let a foot injury keep you on the sidelines. Schedule a foot and ankle consultation with us today, and let's get you back on your feet.
If you have any concerns about your joints, contact us and we can help determine a treatment that works for you.